
Summary
Employers are surrounded by benefits data and dashboards, but data alone doesn’t drive results. Outcomes require connecting insights to intentional action. Learn how a closed loop approach can close the gap between benefits offered and benefits used. Read this blog to understand:
- How claims data helps identify cost drivers
- What it means to engage employees with purpose
- Why employees and employees benefit from the insights to outcomes approach
Across the benefits landscape, organizations are surrounded by dashboards, reports and claims data. However, insights can’t be derived from data trapped in spreadsheets or reviewed in isolation and translated into broad programs that struggle to drive engagement or prove results. At the same time, employers are being inundated with bold promises about solutions powered by artificial intelligence (AI), without clear answers to a fundamental question: How does this actually change outcomes?
The next evolution of benefits strategy isn’t about collecting more data or adopting AI for its own sake. It’s about building a deliberate, closed-loop approach that connects insights to action and action to outcomes. In practical terms, this approach helps close the gap between the benefits offered and the benefits used.
Moving Beyond AI Hype to Purposeful Intelligence
Artificial intelligence has enormous potential in benefits administration and health management, but only when applied with intent. Employers don’t need a single, all-encompassing AI feature. They need the appropriate type of intelligence at the right moment. This means intelligence grounded in high-quality data, governed responsibly and designed to support human decision-making rather than replace it.
An effective insights to outcomes approach treats AI as an enabler across the full lifecycle where it supports the following activities:
- Identifying benefits cost drivers.
- Activating targeted solutions.
- Creating meaningful employee engagement.
- Validating the impact of your benefits strategy.
These four activities create a continuous cycle, with opportunities to optimize the process throughout. Here’s a look at the insights to outcomes approach and why this benefits strategy provides mutual value for employers and their workforce.
Four Steps in the Insights to Outcomes Approach
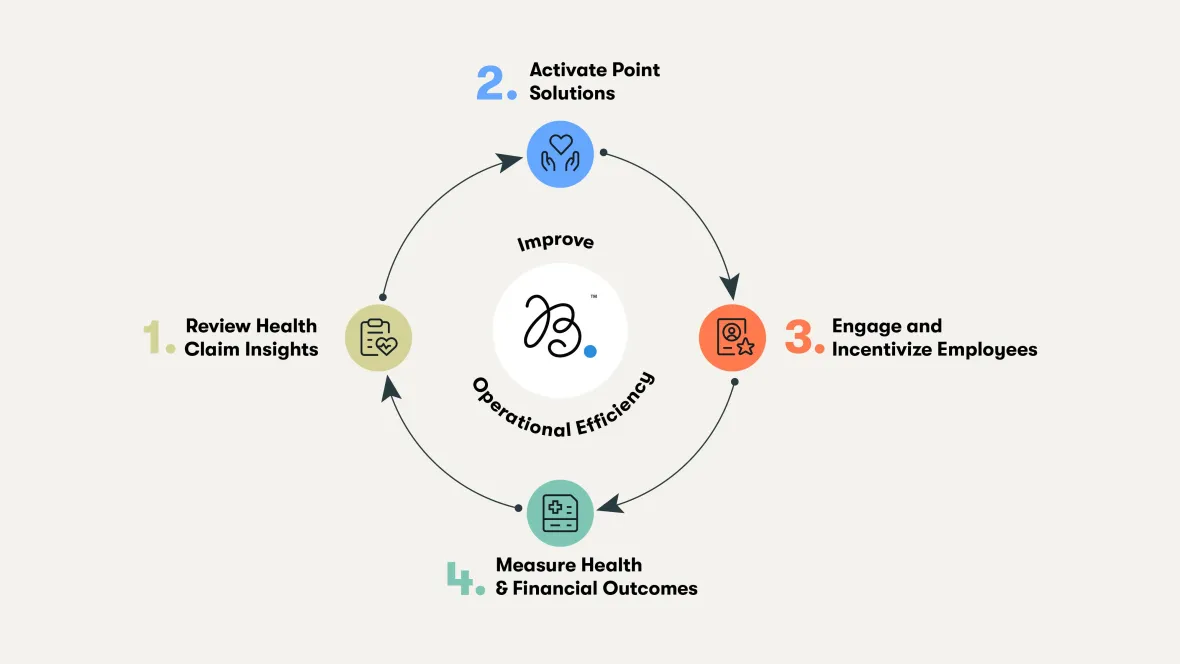
Step 1: Identifying What’s Really Driving Cost
The journey starts with understanding why costs are rising, not just where they appear on a report.
Advanced analytics and machine learning models applied to medical and pharmacy claims data allow employers to move beyond static, backward-looking reporting. By incorporating clinical modeling and historical claims patterns, employers gain visibility into high-cost conditions, emerging trends, and risk segments that warrant attention.
This level of insight creates a stronger foundation for collaboration with consultants and plan partners. Instead of reacting to last year’s spend, employers can focus conversations on predicted utilization patterns and the areas where targeted intervention is most likely to make a difference.
Step 2: Activating Intentional Solutions
Insights only matter if they inform decisions.
When claims intelligence is directly connected to benefits strategy, employers can move away from generic program sprawl and toward more intentional activation. Data-informed insights help employers and consultants evaluate point solutions confidently, prioritize programs aligned to real population needs, and reduce guesswork in benefits design.
Importantly, AI doesn’t replace human judgment in this process. It augments it. Employers remain in control, using intelligence to sharpen focus and align investments to what their population actually needs.
Step 3: Engaging Employees with Purpose
This is where insights truly become outcomes.
When claims insights are integrated with benefits administration, engagement becomes both more personal and more meaningful. Rather than broad, one-size-fits-all communications, employers can guide employees toward relevant actions at the right time. This might mean guiding employees to optimum benefit choices, completing preventive care or engaging at-risk employees with an available point solution.
Personalized nudges, incentives that reinforce behavior change, and intelligent, plan-specific assistance reduce friction and help employees navigate complex benefits decisions. The goal isn’t activity for activity’s sake. It’s engagement with intent, designed to influence behavior and support optimal health and financial outcomes.
Step 4: Measuring Outcomes with Confidence
One of the biggest challenges in benefits strategy is proving what works.
A closed-loop insights to outcomes model uses the same claims data to measure impact that originally identified the opportunity. This allows employers to evaluate results independently, rather than relying solely on vendor-reported metrics.
Ongoing monitoring, interactive reporting, and claims-based ROI analysis provide clearer visibility into utilization, engagement, and financial outcomes. Just as importantly, they make it easier to identify what isn’t working so strategies can be refined rather than repeated blindly.
Optimizing and Repeating the Loop
The final advantage of an insights to outcomes approach is operational efficiency.
When data is used to identify solutions that will make a real impact, partnerships can help make those solutions easy to implement. With targeted employees specifically nudged to use those solutions, employee experiences and benefits usage measurements have the opportunity to become more meaningful.
Over time, this creates a system that learns and improves. Baselines are established, trends tracked and tweaks made to help ensure programs are driving targeted wellness improvements that can decrease future high-cost medical and pharmacy needs.
Why an Insights to Outcomes Approach Matters Now
The value of an insights to outcomes approach extends across the entire organization, creating tangible benefits for employers and employees alike. Among Benefitfocus clients who applied this approach, average medical and prescription spend increased by 2.4%, compared with a reported industry average of 6%.1
For Employers: Smarter Investments, Better Results
Rising healthcare costs make fragmented benefits strategies unsustainable. An insights to outcomes approach helps connect data to action, encouraging employers to focus investments where they drive the greatest impact instead of spreading dollars across generic programs. With independent, claims-based validation, leaders gain clear return on investment (ROI), refine strategies more knowledgably and reduce administrative burden. As a result, benefits teams are free to focus on strategy and adapt to changing workforce needs.
For Employees: Relevant Support When It Matters Most
For employees, an insights to outcomes approach turns benefits into ongoing, personalized support. Instead of generic messages or one‑time enrollment decisions, employees receive timely guidance aligned to their needs, whether they’re preparing for a new baby, managing a chronic health condition or choosing coverage. The goal is less stress, optimal decisions and stronger health and financial wellbeing. Employees don’t just access benefits, they engage with benefits that truly work for them.
Bridging the Gap Between Offering and Impact
The most significant value of an insights to outcomes approach is its ability to close the gap between benefits offered and benefits used. Employers invest substantial resources in comprehensive benefits packages, yet utilization may remain low and outcomes difficult to measure. This disconnect serves no one.
By turning insights into targeted action and measuring results with confidence, organizations have a real opportunity to create a benefits strategy that delivers on its promise. Employers gain control over costs and demonstrate clear value. Employees receive support that improves their lives. And the entire organization benefits from a healthier, more engaged workforce.
The future of benefits isn’t about more dashboards or louder AI claims. It’s about turning insight into action and action into outcomes that are measurable, repeatable, and trusted by everyone involved.
Interested in seeing how an insights to outcomes approach can work in practice? Explore how Benefitfocus connects data, intelligence, and engagement to help employers drive better health and financial outcomes.


